Internship diaries – Cleanest cataract
Cataract surgery is the most common eye surgery to be performed by an ophthalmologist.
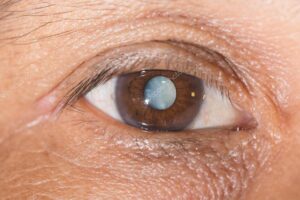
I have seen many cataract surgeries operated by various doctors. I have also read about it extensively and understand the postoperative symptoms well. The important part of examining a post-operative patient on day one is their vision, pressure, anterior and posterior segment evaluation. On slit-lamp examination patients usually have mild congestion in the conjunctiva, corneal oedema and watering. Their symptoms reduce and the vision clears up by the end of 1 week most of the time.
The thought of an ideal cataract post-operative day changed when I came across a patient at another branch of the hospital I worked at. I expected to find similar symptoms and complaints from the patient but I did not find any signs of inflammation. I rechecked the patient’s records to confirm the cataract surgery was performed otherwise I couldn’t believe it. The cornea consultant there performed surgery using a scleral incision due to which the cornea is not touched at all. Until that day I used to think I knew all about cataracts but this doctor showed how beautiful a cataract surgery can be! The patient did not have any complaints or symptoms at all!
When I need cataract surgery I would find a doctor like her! That’s how much I loved it.
For another interesting internship diaries click on Lacrimal syringing-the worst nightmare of the interns